COVID-19 Dashboard
THE PROBLEM
Hill-Burton Modernization and Construction Act in 1946 funded the construction of an average of 4 to 5 hospital beds per 1,000 people across the United States. It permitted the distribution of funds on a per capita basis tied to income. After the Civil Rights Act passed, hospitals began to desegregate. More people moved to the suburbs, and fewer people were in urban and rural areas. Urban and rural bed occupancy rates declined by double digits between the 1940s and 1970s. In response, health planners began to cut hospital beds, which was called “hospital cost containment. By cutting inpatient beds and redirecting those resources to outpatient care to increase profitability. This reduced hospital surge capacity. The reduction of inpatient hospital beds has been happening since the 1970s.
It is suspected that communities of color in 2020 have access to fewer hospital beds than white people. Also, wealthier neighborhoods will have more hospital beds to deal with COVID19 than more impoverished communities.
The goal is to build awareness of factors that COVID19 trajectory in communities of color. Also, I sought to provide data visualization to identify opportunities to improve health in the United States.
THE SOLUTION
Using Python and Tableau, I built a dashboard that automatically takes data from covidtracking.com and displays it on a dashboard with Census and Kaiser Family Foundation data. With this dashboard, you can see which states have the least total beds per capita and least ICU beds per capita. Along with state-level data on which race was most heavily impacted by COVID19 in that particular state.
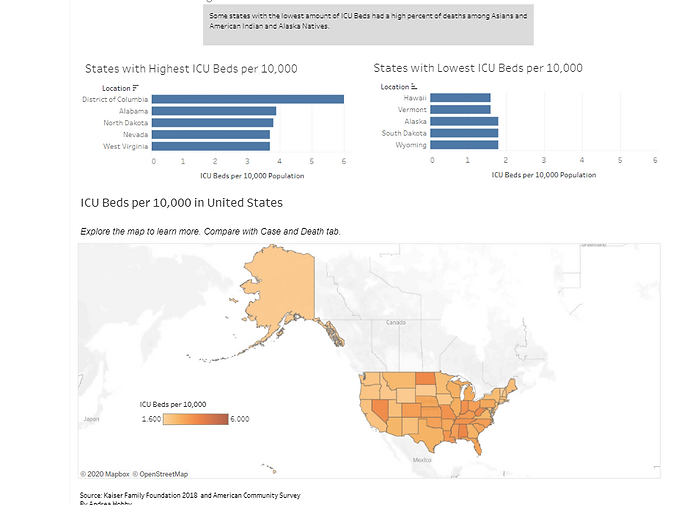
RESULTS
States like New Mexico and Wyoming have many deaths in American Indian and Alaska Native populations than other states. Also, African Americans have a significant share of deaths in Maryland, Louisiana, and DC than other states. I want to go further with county-level data. If county-level race data for cases and deaths were available, I think this would be more revealing.
PROJECT WEBSITE
For more details, check out the project’s website here.